- Latest news▼
-
18:22, April 17 First Armenian-German Conference entitled “Heart Failure Spring School”

-
14:37, April 16 Daily Mail: intermittent fasting is not suitable for children and women before their periods

-
16:41, April 15 Cell: in carriers of defective BRCA2 gene, sugar consumption increases cancer risk

-
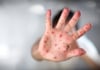
15:04, April 15 305 cases of measles recorded in Armenia so far in 2024
-
14:38, April 15 Food and Environmental Virology: tea contributes to effective coronavirus control

-
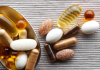
12:41, April 15 Daily Mail: vitamin A, B3 and E supplements can be dangerous
-
10:56, April 15 Diabetes Care: evening physical activity is good for the heart

-
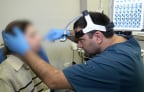
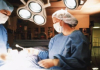
08:27, April 15 Women are more susceptible to blood loss and death during bypass surgery than men, researchers say
-
18:42, April 13 WHO: Nigeria pioneers revolutionary meningitis vaccine
-
16:43, April 13 One-third of women experience menstruation-related migraines, most often during premenopause - study

-
14:37, April 12 Pediatrics: Hypoglossal nerve stimulation implant helps with sleep apnea

-
12:13, April 12 Health minister: Simulation educational center will be created, assisted reproductive technology capacity will increase in Armenia

-
17:03, April 11 BMJ: antidepressant injection 4 times reduced risk of severe postpartum depression

-
11:35, April 11 Health minister: Number of hard-to-reach medical services within state funding scope increased in Armenia in 2023

-
16:10, April 10 Breathing therapy, which is so popular in the world, is starting to spread in Armenia

All materials
Researchers find women make better surgeons than men

In a new study published in the BMJ, researchers asked that very question. Surgery has long been a male-dominated occupation: first because few women enrolled in medical school, and then because they weren't perceived (by male surgeons, no less) to have the temperament needed to make the life-and-death decisions required in an OR. But in the latest report, it turns out that the patients of female surgeons tend to have lower death rates, fewer complications and lower readmissions to the hospital a month after their procedure, compared to the patients of male surgeons.
The study included all of the people in Ontario, Canada who had operations from 2007 to 2015 (more than 104,000, in total) as well as their surgeons. Dr. Raj Satkunasivam, assistant professor of urology at Houston Methodist Hospital and leader of the study, and his colleagues went to great lengths to equalize the comparisons between the male and female surgeons. Since surgery is a field in which experience can lead to better outcomes, they matched the surgeons by age and experience. They also matched the patients of each surgeon as much as possible to account for the fact that some surgeons might have had more difficult and complicated cases.
Even after those adjustments, patients of female surgeons were 4% less likely to die, be readmitted or experience complications 30 days after their surgery compared to patients of male surgeons.
This is not the first time a study has found that a doctor's gender may influence patient outcomes. In a study earlier this year, other researchers from the Harvard School of Public Health looked at a group of patients seeing general internists and found that those with female doctors tended to have lower death rates and were less likely to be readmitted to the hospital within 30 days than those with male doctors. The authors attribute the favorable patient outcomes to the female doctors' ability to communicate and engage with their patients to ensure compliance with medications and therapy, their adeptness at collaborating with colleagues and their tendency to adhere to guidelines when treating patients.
But there have not been many studies looking at the role of gender in surgery outcomes, so it’s not clear why the patients of female surgeons might do better than those of male surgeons. The same factors that might contribute to female internists having better outcomes for their patients could also play a role among surgeons. But there are likely other contributors involved as well, since surgery is typically dependent on the skill of the surgeon and his or her ability to assess a person's likelihood of surviving or developing complications.
One such factor, Satkunasivam says, is that generally only the very best women at the craft become practicing surgeons. Because surgery has traditionally been a male-dominated field in medicine, the female surgeons operating now have likely had to overcome higher barriers in order to rule the operating room. Therefore, the female surgeons in the study may have been a select group of the gender’s best. Still, the data are compelling enough that they deserve to be repeated and investigated further.
“If we really believe that the differences we saw among male and female surgeons is true, then what we need to do is better understand what actually is driving those differences,” says Satkunasivam. “Once we understand those differences, we can potentially apply them to train surgeons better, and instill those qualities in all surgeons to improve outcomes for everyone.”In the meantime, he says, gender shouldn’t be a factor in deciding which surgeon should be in charge of your next operation. “You should select a surgeon based on the rapport you have with him or her, what your family physician recommends, and the research you do,” says Satkunasivam. “You should be equally confident with a male or female surgeon.”
Follow NEWS.am Medicine on Facebook and Twitter
- Video
- Event calendar
- Archive
- Most read
month
week
day
- BMJ: antidepressant injection 4 times reduced risk of severe postpartum depression 1459
- Pediatrics: Hypoglossal nerve stimulation implant helps with sleep apnea 1312
- Health minister: Simulation educational center will be created, assisted reproductive technology capacity will increase in Armenia 1276
- WHO: Nigeria pioneers revolutionary meningitis vaccine 1114
- One-third of women experience menstruation-related migraines, most often during premenopause - study 1090
- Women are more susceptible to blood loss and death during bypass surgery than men, researchers say 781
- Food and Environmental Virology: tea contributes to effective coronavirus control 765
- Daily Mail: vitamin A, B3 and E supplements can be dangerous 764
- 305 cases of measles recorded in Armenia so far in 2024 728
- Cell: in carriers of defective BRCA2 gene, sugar consumption increases cancer risk 725
- Diabetes Care: evening physical activity is good for the heart 717
- Daily Mail: intermittent fasting is not suitable for children and women before their periods 544
- First Armenian-German Conference entitled “Heart Failure Spring School” 323
- Find us on Facebook
- Poll