- Latest news▼
-
15:11, April 24 Zombie deer disease possibly linked to hunters’ deaths

-
12:27, April 23 Appetite: Scientists found out the secret to the appeal of large portions of fast food

-
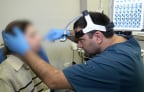
10:33, April 23 Scientists test new approach to fighting viruses

-
08:38, April 23 Ketamine may help with postpartum depression

-
22:12, April 22 Unhealthy amount of sugar found in baby food products of a well-known brand

-
19:41, April 22 Air pollution puts health of more than 1.6 billion workers globally at risk

-
17:25, April 22 Scientists found baked goods and lack of sleep to be more dangerous than alcohol

-
16:02, April 22 342 cases of measles recorded in Armenia so far in 2024
-
15:29, April 22 BrainStimulation: electrical brain stimulation alleviates anxiety and depression in the elderly

-
08:27, April 22 Cognitively stimulating jobs in midlife could lower dementia risk in old age, study finds

-
20:37, April 21 Environmental Health Perspectives: Microplastics ingested with food and water can spread from the gut to the brain

-
22:41, April 20 Scientists develop new method to safely stimulate immune cells to fight cancer

-
20:46, April 20 Blood test can determine who is at risk of developing multiple sclerosis - scientists

-
18:36, April 20 Next pandemic likely to be triggered by flu - scientists

-
12:16, April 19 Scientists grow human mini-lungs in lab

All materials
Viruses show new promise in treating cancer
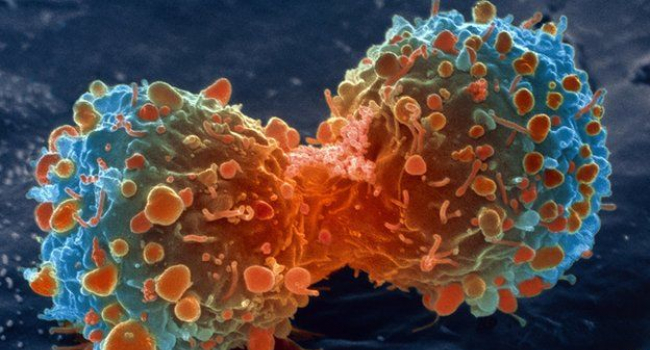
Viruses have shown renewed promise in the treatment of cancer, after new research has shown they retain their cancer-killing ability even when injected into the bloodstream.
The discovery could see viruses used to treat many more patients and a wider range of cancer types than it was previously thought possible.
It is believed that the human body's normal immune response neutralizes viruses that are injected into the bloodstream to try to destroy cancer tumours, during virus therapy.
In a new study investigating reovirus, scientists found that cells in the blood can reactivate the virus as it travels to the tumour site, allowing it to retain its ability to destroy the cancer cells.
Viruses generally attack the body and cause harm, but some viruses specifically target and destroy cancer tissue while causing minimal side effects to the patient, making them an attractive new type of cancer treatment, known as oncolytic virus therapy.
A type of virus, called T-vec, is approved on the NHS for advanced melanoma skin cancers and is given to patients by injection directly into their tumours – but this means the tumours have to be somewhere in the body that can be reached with a needle.
Patients receiving injections of virus therapy into the bloodstream in clinical trials quickly developed antibodies which could potentially deactivate the virus, and this was previously believed to stop it functioning.
However, new research shows that white blood cells, which can carry the virus to the tumour site, can also reactivate these deactivated viruses, allowing them to infect and kill the cancer cells.
The study, published in the journal Cancer Immunology Research, was led by Dr. Elizabeth Ilett and Dr. Rob Berkeley from the University of Leeds and Professor Alan Melcher from the Institute of Cancer Research, London.
Dr. Ilett, from the Leeds Institute of Cancer and Pathology at the University, said: "This discovery suggests that cancer treatments using virus therapy could be significantly expanded in future, as we previously believed that follow-up doses were useless once the body had produced antibodies against the virus.
"We are only just beginning to understand how viruses can help us tackle cancer, but it is exciting to learn that our bodies are actually capable of helping them to destroy cancer tumours."
Using antibodies from patients undergoing virus therapy, the researchers neutralized viruses and added them to melanoma cells in the laboratory, which on its own had no effect. But adding white blood cells, called monocytes, meant the virus became reactivated, allowing it to destroy the cancer cells.
The study looked at three different viruses which are currently being used in clinical trials, and found that neutralized forms of two of the three viruses could be reactivated by white blood cells. The authors believe it is therefore likely that other viruses might also be effective even after being neutralized by antibodies, a finding with immediate clinical significance.
Co-lead author Professor Melcher, said: "Viruses are a hugely exciting new type of treatment for cancer. Not only do virus therapies kill cancer cells directly, they do so with only mild side effects compared to traditional cancer treatments and they attract the immune system to the site of the tumour – which means they can work well when combined with other types of immunotherapy.
"At present, these cancer-killing viruses work really well when injected directly into the site of a tumour – but that means the tumour has to be somewhere in the body that you can reach with a needle.
"Our study shows that, crucially, viruses retain their cancer-killing ability even in the bloodstream. This research has profound implications for how we might use viruses to treat cancer in future, opening up virus therapy to many more patients with hard-to-reach tumours of different cancer types."
Currently, a number of viruses are being tested in clinical trials, but only one virus has been approved for general use, by injection directly to the tumour. The researchers hope that this study will help us gain a better understanding of how virus therapies work, so that they can be used in combination with other immunotherapies in future.
Follow NEWS.am Medicine on Facebook and Twitter
- Video
- Event calendar
- Archive
- Most read
month
week
day
- JAMA Oncology: Urine test can help rule out high-grade prostate cancer with almost 100% accuracy, study shows 1243
- Daily Mail: Elderly woman in China gets infected with brain-eating amoeba 1188
- Obesity: exercising before breakfast helps you lose weight faster 1169
- The Conversation: childhood trauma can cause pathological hoarding 1164
- Scientists grow human mini-lungs in lab 1135
- Next pandemic likely to be triggered by flu - scientists 844
- Scientists found baked goods and lack of sleep to be more dangerous than alcohol 763
- 342 cases of measles recorded in Armenia so far in 2024 721
- Blood test can determine who is at risk of developing multiple sclerosis - scientists 702
- Scientists develop new method to safely stimulate immune cells to fight cancer 699
- Cognitively stimulating jobs in midlife could lower dementia risk in old age, study finds 685
- BrainStimulation: electrical brain stimulation alleviates anxiety and depression in the elderly 632
- Air pollution puts health of more than 1.6 billion workers globally at risk 499
- Unhealthy amount of sugar found in baby food products of a well-known brand 491
- Ketamine may help with postpartum depression 475
- Find us on Facebook
- Poll