- Latest news▼
-
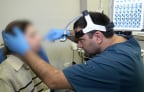
12:16, April 19 Scientists grow human mini-lungs in lab

-
10:23, April 19 JAMA Oncology: Urine test can help rule out high-grade prostate cancer with almost 100% accuracy, study shows

-
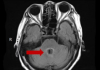
18:00, April 18 Daily Mail: Elderly woman in China gets infected with brain-eating amoeba
-
14:19, April 18 Obesity: exercising before breakfast helps you lose weight faster

-
10:42, April 18 The Conversation: childhood trauma can cause pathological hoarding

-
08:37, April 18 Daily Mail: Satiating food reduces cravings for sweets, nutritionist says

-
18:22, April 17 First Armenian-German Conference entitled “Heart Failure Spring School”

-
08:38, April 17 Why do kids usually recover from COVID-19 more easily than adults?

-
14:37, April 16 Daily Mail: intermittent fasting is not suitable for children and women before their periods

-
16:41, April 15 Cell: in carriers of defective BRCA2 gene, sugar consumption increases cancer risk

-
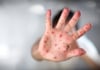
15:04, April 15 305 cases of measles recorded in Armenia so far in 2024
-
14:38, April 15 Food and Environmental Virology: tea contributes to effective coronavirus control

-
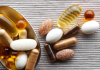
12:41, April 15 Daily Mail: vitamin A, B3 and E supplements can be dangerous
-
10:56, April 15 Diabetes Care: evening physical activity is good for the heart

-
08:27, April 15 Women are more susceptible to blood loss and death during bypass surgery than men, researchers say
All materials
Breast cancer drug given to hundreds of thousands of women on the NHS affects brain function and memory

A drug commonly given out by the NHS to breast-cancer patients may affect their brain function and memory, research suggests.
Letrozole is primarily used to treat breast cancer and was prescribed 755,866 times last year in the UK, NHS Digital statistics show.
Although Cancer Research UK states up to 30 per cent of patients experience side effects like hot flushes and fatigue, new research suggests the medication's complications may be far more serious.
When given to monkeys, the drug reduced the function of their brain cells in a region known as the hippocampus, and worsened their performance on memory tests, after just four weeks.
The study was carried out by the University of Toronto and led by research associate Dr Nicole Gervais.
Some breast cancers are stimulated by the hormone oestrogen, which may get converted from testosterone via the enzyme aromatase. Letrozole - which is given as a tablet - is an aromatase inhibitor (AI).
Letrozole only works in women with this form of breast cancer who have been through the menopause. This is due to them no longer producing oestrogen via their ovaries, with the hormone therefore only coming about via aromatase.
The drug is linked to joint pain and raised cholesterol levels in one in ten people, as well as loss of appetite, hair thinning and vaginal dryness in one per cent of cases. It is often given after surgery or chemo to prevent cancer returning or spreading.
Letrozole may bring about depression, forgetfulness and insomnia due to aromatase being expressed in the hippocampus, which is the brain region that controls emotion, memory and thought processing.
'Four weeks of an oral AI has adverse effects on multiple behavioral, neuronal and physiological outcomes in marmosets,' the authors wrote in The Journal of Neuroscience.
In the first study of its kind, three male and five female marmoset monkeys were fed letrozole - also known by its brand name Femara - hidden in pudding. The amount given was calculated 'based on the recommended dose for women'.
These monkeys were compared against six males and two females who were just fed the pudding.
Marmosets were chosen due to the 'organisation of the brain being comparable to a human's', the authors wrote. The monkeys also 'share many similarities with humans in sleep, cognitive ability and anxiety profiles'.
Urine samples from the animals were analysed to determine levels of the stress hormone cortisol. Signs of anxiety were also monitored in the animals' behaviour, such as their 'hair standing on end' or any agitated movements.
When the experiment ended, the monkeys were put down so changes to their brain structure could be analysed.
Results suggest the animals given letrozole had reduced brain cell activity in the hippocampus and performed worse on memory tests.
The letrozole group demonstrated a drop in performance of five to seven per cent, however it is difficult for the authors to interpret how meaningful this change would be.
They also spent more time acting agitated and had higher facial temperatures - a sign of hot flushes.
While the link between these symptoms, including effects to the brain, and the use of aromatase inhibitors has been made before, it's the first time a clear direct link has been made.
Dr Gervais told MailOnline: 'Women have also been treated with chemotherapy, radiation thereapy and other anti-estrogen medications with known effects on the brain, and so it has been a challenge to tease apart the unique contributions of aromatase inhibitors to the reported side effects.'
Although the findings can't be applied to women in general, Dr Gervais said: 'They can inform women considering taking this medication about what some of the effects might be.
'These findings might also help normalize some of the experiences women currently taking the medication are having.'
Although concerning, the researchers stress further studies are required and letrozole has been shown to boost survival among breast-cancer patients.
Five-year disease-free survival was higher in a group treated with letrozole - at 95 per cent - compared with 91 per cent among a placebo group, researchers at the Avon International Breast Cancer Research Program at Massachusetts General Hospital Cancer Center found.
Breast cancer is the most common cancer in women worldwide, with nearly 1.7million new cases diagnosed in 2012, according to the World Cancer Research Fund.
It even affects one in eight women at some point in their lives in both the US and UK.
Source: The Daily Mail
Follow NEWS.am Medicine on Facebook and Twitter
- Video
- Event calendar
- Archive
- Most read
month
week
day
- WHO: Nigeria pioneers revolutionary meningitis vaccine 1190
- One-third of women experience menstruation-related migraines, most often during premenopause - study 1188
- Daily Mail: vitamin A, B3 and E supplements can be dangerous 1083
- Food and Environmental Virology: tea contributes to effective coronavirus control 1075
- Cell: in carriers of defective BRCA2 gene, sugar consumption increases cancer risk 1046
- 305 cases of measles recorded in Armenia so far in 2024 1040
- Women are more susceptible to blood loss and death during bypass surgery than men, researchers say 974
- Diabetes Care: evening physical activity is good for the heart 929
- Daily Mail: intermittent fasting is not suitable for children and women before their periods 870
- First Armenian-German Conference entitled “Heart Failure Spring School” 639
- Obesity: exercising before breakfast helps you lose weight faster 538
- Why do kids usually recover from COVID-19 more easily than adults? 538
- Daily Mail: Elderly woman in China gets infected with brain-eating amoeba 529
- The Conversation: childhood trauma can cause pathological hoarding 526
- Daily Mail: Satiating food reduces cravings for sweets, nutritionist says 501
- Find us on Facebook
- Poll