- Latest news▼
-
12:27, April 23 Appetite: Scientists found out the secret to the appeal of large portions of fast food

-
10:33, April 23 Scientists test new approach to fighting viruses

-
08:38, April 23 Ketamine may help with postpartum depression

-
22:12, April 22 Unhealthy amount of sugar found in baby food products of a well-known brand

-
19:41, April 22 Air pollution puts health of more than 1.6 billion workers globally at risk

-
17:25, April 22 Scientists found baked goods and lack of sleep to be more dangerous than alcohol

-
16:02, April 22 342 cases of measles recorded in Armenia so far in 2024
-
15:29, April 22 BrainStimulation: electrical brain stimulation alleviates anxiety and depression in the elderly

-
08:27, April 22 Cognitively stimulating jobs in midlife could lower dementia risk in old age, study finds

-
20:37, April 21 Environmental Health Perspectives: Microplastics ingested with food and water can spread from the gut to the brain

-
22:41, April 20 Scientists develop new method to safely stimulate immune cells to fight cancer

-
20:46, April 20 Blood test can determine who is at risk of developing multiple sclerosis - scientists

-
18:36, April 20 Next pandemic likely to be triggered by flu - scientists

-
12:16, April 19 Scientists grow human mini-lungs in lab

-
10:23, April 19 JAMA Oncology: Urine test can help rule out high-grade prostate cancer with almost 100% accuracy, study shows

All materials
Novel implant to protect women from HIV infection
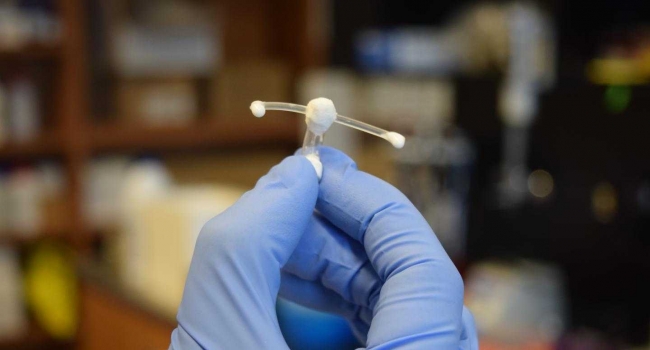
Scientists have developed a vaginal implant that can protect women from HIV infection by decreasing the number of cells that the virus can target in their genital tract.
Unlike conventional methods of HIV prevention, such as condoms or anti-HIV drugs, the implant takes advantage of some people's natural immunity to the virus, according to researchers at the University of Waterloo in Canada.
The implant, described in the Journal of Controlled Release, is composed of a hollow tube and two pliable arms to hold it in place.
It contains hydroxychloroquine (HCQ) which is disseminated slowly through the porous material of the tube and absorbed by the walls of the vaginal tract.
"We know that some drugs taken orally never make it to the vaginal tract, so this implant could provide a more reliable way to encourage T cells not to respond to infection and therefore more reliably and cheaply prevent transmission," said Emmanuel Ho, a professor at the University of Waterloo.
"What we do not know yet is if this can be a stand-alone option for preventing HIV transmission or if it might be best used in conjunction with other prevention strategies," said Ho.
HIV infects the body by corrupting T cells that are mobilised by the immune system when the virus enters a person's body.
When the T cells stay resting and do not attempt to fight the virus they are not infected and the HIV virus is not transmitted between people. When the T cells stay resting, it is referred to as being immune quiescent.
The implants were tested in an animal model and the team observed a significant reduction in T cell activation, meaning that the vaginal tract was demonstrating an immune quiescent state.
The new implant was inspired by previous research involving sex workers in Kenya.
In Kenya, Ho and research partner Keith Fowke of the University of Manitoba, observed that many of these women who had sex with HIV positive clients but did not contract the virus.
They later found the women possessed T cells that were naturally immune quiescent.
"Observing this, we asked ourselves if it was possible to pharmacologically induce immune quiescence with medication that was better assured of reaching the point of infection," said Ho.
"By delivering the medication exactly where it is needed, we hoped to increase the chances of inducing immune quiescence," he said.
Follow NEWS.am Medicine on Facebook and Twitter
- Video
- Event calendar
- Archive
- Most read
month
week
day
- JAMA Oncology: Urine test can help rule out high-grade prostate cancer with almost 100% accuracy, study shows 1172
- Daily Mail: Elderly woman in China gets infected with brain-eating amoeba 1148
- Obesity: exercising before breakfast helps you lose weight faster 1133
- The Conversation: childhood trauma can cause pathological hoarding 1131
- Daily Mail: Satiating food reduces cravings for sweets, nutritionist says 1105
- First Armenian-German Conference entitled “Heart Failure Spring School” 1054
- Why do kids usually recover from COVID-19 more easily than adults? 1002
- Scientists grow human mini-lungs in lab 995
- Next pandemic likely to be triggered by flu - scientists 548
- Scientists found baked goods and lack of sleep to be more dangerous than alcohol 486
- Blood test can determine who is at risk of developing multiple sclerosis - scientists 447
- Scientists develop new method to safely stimulate immune cells to fight cancer 442
- 342 cases of measles recorded in Armenia so far in 2024 431
- Cognitively stimulating jobs in midlife could lower dementia risk in old age, study finds 422
- BrainStimulation: electrical brain stimulation alleviates anxiety and depression in the elderly 358
- Find us on Facebook
- Poll